髋关节疾病及治疗策略2021年进展:美国运动医学杂志综述
2022-03-25 文章来源:Am J Sports Med 作者:译者:陶可 我要说
作者:Bruce Reider
作者单位: Chicago, Illinois
译者:陶可(北京大学人民医院骨关节科)
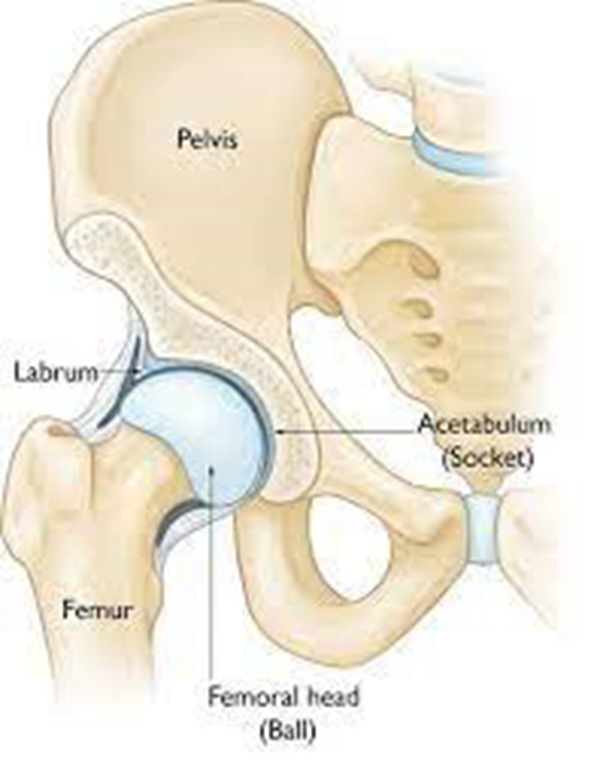
图1 正常髋关节是由髋臼(球窝)与股骨头(球体)以及覆盖在其表面的软骨、围绕在周围的盂唇、小凹韧带、关节囊、髋周肌肉、血管神经等组成复杂的复合体。发挥联接骨盆与以上身体重量传递至下肢股骨的桥梁作用。因为各种原因,如饮酒、激素、外伤股骨头/股骨颈骨折后等,可导致股骨头无菌性/缺血性骨坏死(股骨头坏死)、先天性或继发性髋臼发育不良、髋关节结核/细菌感染等所致的髋关节融合、盂唇损伤、髋臼股骨头颈部撞击症、坐骨股骨撞击症、复杂髋关节/股骨头颈部畸形;Perthes病等均会影响髋关节功能,轻者可能出现反复或持续性髋关节周围酸胀疼痛、重者可能出现跛行或无法站立行走;且髋关节疾病很容易与腰骶部病变、骶髂关节炎症、梨状肌综合征、坐骨结节滑囊炎、腰椎间盘突出症等相混淆,需细致且准确的临床查体、影像学检查,如X线片、彩超、CT扫描、及核磁共振检查,以明清病因。
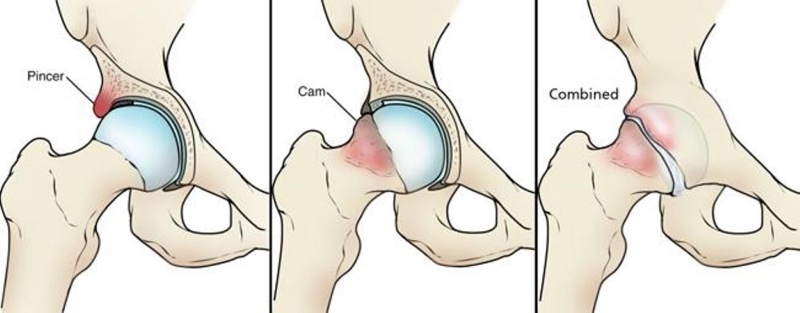
图2 髋臼股骨头颈部撞击症FAI分为3种:钳夹型撞击、凸轮型撞击以及两者均存在的混合型撞击。
图3 髋关节镜通过微创手术入路,可以实现对股骨头颈部撞击症FAI、盂唇损伤、脂肪变性、滑膜炎、游离体、小凹韧带撕裂等的有效处理。

如果一位报纸记者要我找出21世纪头20年间骨科运动医学领域的重大事件,我必须带头推荐髋关节镜检查和相关关节保留技术的巨大发展。仅在20年前,您可能一方面指望以髋关节镜检查专业知识而闻名的北美外科医生的数量,并且可以说他们有能力满足非洲大陆对这种技术的需求。今天,髋关节镜检查仍然足以引起专业人士的兴趣,以至于其从业者经常专注于这一关节,但他们的数量在世界范围内呈指数增长。髋关节镜检查已成为骨科运动医学访学课程不可或缺的一部分。这种增长的功劳必须由有见地的外科医生分享,他们将股骨髋臼撞击征(FAI)确定为疼痛和髋关节退化(骨关节炎)的原因,以及那些利用他们的创造力将关节镜技术应用于其治疗的人。这种独创性使得髋臼盂唇的手术治疗从简单的清创到修复再到重建的速度惊人地增长。本月《美国运动医学杂志》上的一系列论文展示了当代髋关节镜临床研究的多样性。
这些文章的第一篇通过记录Minnesota, Olmsted明尼苏达州奥姆斯特德县2000年至2016年股骨髋臼撞击征(FAI)的诊断和治疗,反映了21世纪髋关节镜检查的发展。这个县在2010年拥有144,260人口,有幸成为著名的Mayo梅奥诊所和Rochester罗切斯特流行病学项目的所在地。该项目将所有奥姆斯特德居民的医疗记录联系起来,无论他们在哪里获得医疗保健。本研究的作者确定了1893名14至50岁的患者,他们在2000年至2016年期间从奥姆斯特德医生那里接受了髋部疼痛、髋部撞击或髋关节疾病的诊断。在检查了患者的记录和X线片后,研究人员确定716名患者的813髋符合股骨髋臼撞击征(FAI)的Warwick标准。在整个期间,股骨髋臼撞击征(FAI)的发生率为54.4/100,000人年:女性(73.2)高于男性(36.1)。一个重要的观察结果是,诊断的发生率随着时间的推移而增加,从2000-2004年的每10万人年40.3例增加到2005-2009年的45.3例,再到2010-2016年的72.6例。正如作者所观察到的,对于股骨髋臼撞击征(FAI)明显增加的最可能的解释是对这种情况的日益认识,而不是其发生的真正爆炸式增长。尽管非手术治疗是最常见的治疗方法,但在研究期间手术治疗的频率随之增加。最引人注目的是,关节镜治疗的使用从2000-2004年的1例增加到2010-2016年的160例。
正如股骨髋臼撞击征(FAI)和其他髋关节疾病的识别和治疗在过去20年中已经成熟一样,相关研究也蓬勃发展。早期的报告通常是案例系列,后续研究出人意料地简短,因为从业者努力将他们的初步结果付诸发表。近年来,这些已经让位于2、5甚至10年随访的比较研究。随机试验现在出现的频率越来越高。在本期AJSM中,FIRST研究小组的成员报告了一项有影响的跨国试验的2年结果,该试验旨在确定骨软骨成形术是否为接受关节镜下盂唇治疗以治疗疼痛的非关节炎股骨髋臼撞击征(FAI)的患者提供额外的益处。研究人员随机分配了220名患者对照组,根据需要接受关节镜灌洗和盂唇修复,以及骨软骨成形术组,其中除了盂唇修复外,还切除了凸轮型和钳夹型撞击病变。
本研究的结果可能有助于深入了解髋臼盂唇损伤的发病机制。当作者分析术后12个月的视觉模拟评分(VAS)疼痛测量的主要结果时,治疗组之间没有显着差异。12个月功能评分的次要结果也没有差异,除了对照组一个指标优于治疗组。然而,与对照组(19/104)相比,骨软骨成形组(8/105)的24个月再手术率(主要是疼痛或盂唇再损伤)显着降低:优势比,0.37(95% CI,0.15-0.89)。
由于两组在12个月时报告的疼痛水平没有差异,我们可以推断关节镜治疗股骨髋臼撞击征(FAI)后最初的疼痛缓解可能归因于盂唇修复和灌洗的效果。对照组的再手术率增加,最早可在术后2年检测到,这可能被解释为间接证据表明股骨髋臼撞击征(FAI)的骨异常特征是易出现盂唇损伤,并引起疼痛,如果潜在的骨性损伤手术时没有被纠正/处理,这类(FAI基础上的)盂唇损伤可能会再次复发。
在本期AJSM中对10名凸轮型股骨髋臼撞击征(FAI)患者的髋部进行的离散元素分析支持了这一理论。这些作者计算了模拟撞击期间增加的峰值关节接触应力与对照髋相比,在有凸轮畸形的髋关节中进行测试。在充分切除凸轮后,峰值接触应力恢复到正常范围。
FIRST试验结果的这种解释得到了Domb等人最近发表的另一篇AJSM文章的支持。在该回顾性队列研究中,作者根据其术前和术后α角测量值将髋关节镜检查患者分为3个匹配组:术前术后α角均为50°,术前α角为55°,术后α角为50°,术前术后α角均为55°。手术时,两组术前α角较大(平均为66°-69°)的盂唇和髋臼软骨损伤均高于术前α角平均仅为50°的第三组。术后至少2年随访时,术前α角较大而未在手术中矫正的组不太可能达到改良哈里斯髋关节评分(mHHS)的患者可接受症状改善状态(PASS),并且比其他2组更可能进展为髋关节置换。
正如Domb等人的这项研究专注于股骨形态的矫正一样,Johannsen等人在本月的AJSM中进行的另一项研究检查了髋臼形态的手术治疗可能如何影响最终结果。在这项研究中,作者报告了192名接受髋臼成形术和盂唇修复术的患者的至少5年的术后结局。患者根据髋臼切除深度进行分类,通过外侧中心边缘角(LCEA)的变化和术后外侧中心边缘角(LCEA)的大小来衡量。与Domb研究相比,这组作者发现这些髋臼形态变化的测量与患者报告结果测量(PROM)定义的临床结果或手术后平均6.5年的翻修率几乎没有关系,这不一定是矛盾的,因为Domb等的研究着眼于(盂唇)切除不足的可能影响,而Johannsen等的研究侧重于分析(盂唇)过度切除的尺寸大小。从逻辑上讲,一定程度的髋臼过度切除会对患者的预后产生不利影响,但作者显然避免了这种过度的髋臼成形术,至少在所选择的结果测量中可以检测到。最后,正如作者所指出的,外侧中心边缘角(LCEA)是最常见的髋臼形态指标,但可能是对影响稳定性或撞击的复杂髋臼因素的过度简化。
这两项研究旨在确定外科手术的细节如何影响最终的治疗结果。许多其他临床髋关节镜研究试图确定可能预测手术结果的其他因素,包括一般患者特征、术前髋关节解剖、术前或术后早期疼痛或患者报告结果测量(PROM)水平。这些研究中的大多数在设计上是回顾性的,因此他们确定了需要在未来的前瞻性研究中验证为真正具有预测性的关联。据报道,正如纽约Yankee伟大的Yogi Berra所说“很难做出预测,尤其是关于未来的预测。”
本月AJSM中的四篇论文研究了患者特征与随后的手术结果之间可能存在的关联。在其中的第一个中,Menge等报告了一组60名青少年在关节镜下治疗股骨髋臼撞击征(FAI)并进行相关的盂唇修复后的结果。术后10年,研究人员注意到10%的翻修率,所有病例均涉及女性患者,这与整体髋关节囊松弛和术前症状持续时间显着相关。在第二项研究中,Lin等人13报告109名患者的5年生存率为71%,失败定义为翻修手术或进展为关节置换术。当他们将患者分为15-34岁、35-50岁和51-75岁的人群时,研究人员发现,年龄最大的人群进行关节置换术的可能性增大了5倍。
除了年龄,Lin等还发现患者的体重指数(BMI)与5岁时的非关节炎髋关节评分(NAHS)和mHHS之间存在关联。Parvaresh及其同事在本月的AJSM上发表的第三篇论文专门关注了患者的BMI与关节镜治疗FAI的5年结果之间的关系。研究人员根据标准定义将140名患者分为正常、超重、肥胖和病态肥胖亚组。尽管所有BMI组的疼痛水平都有显着改善,与正常体重指数BMI组相比,但病态肥胖组不太可能达到患者报告结果测量(PROM)的最小临床重要差异(MCID),所有3个较重的组都不太可能达到PASS和实质性临床益处(SCB)。这组研究中的第四项研究“髋关节镜检查后临床结果的预测因素”由Domb等发现,在一系列860名患者中,除其他因素外,年龄和体重指数BMI与2年和5年结果评分以及转为关节置换术相关。
除了检查性别、全身松弛、年龄和体重指数BMI等一般患者特征外,还进行了许多研究来确定与手术成功或失败相关的髋关节解剖学方面。在另一项研究中本月的AJSM,Maldonado等研究了术前髋臼过度覆盖对股骨髋臼撞击征(FAI)关节镜治疗结果的可能影响。作者比较了45名术前外侧中心边缘角LCEA为40°的患者与年龄、性别、体重指数BMI和随访时间相匹配但外侧中心边缘角LCEA介于25°和40°之间的相似数量的患者的结果。术后5年,两组在几个患者报告结果测量PROM上的平均改善相似,达到最小临床重要差异MCID的比率也相似。有趣的是,过度覆盖组实际上转换为关节置换术的比率较低,尽管作者承认这可能是由于他们的组规模相对较小而导致的I型错误。
Maldonado和许多相同的作者还进行了一项研究,比较了20名临界髋关节发育不良患者(定义为18°和25°之间的外侧中心边缘角LCEA)与61名匹配的对照,其外侧中心边缘角LCEA测量值在25°和40°之间。15 在这项研究中,患者正在接受翻修手术,随访仅2年。同样,两组都报告了患者报告结果测量PROM的类似改善,但对照组在记录的3个患者报告结果测量PROM中的2个上实现最小临床重要差异MCID的比率更高。额外的关节镜翻修率和转为关节置换术的比率也存在差异,这些差异在临床上很重要,但在所研究的样本量中没有统计学意义。
患者和外科医生都想知道他们在髋关节镜检查后的早期结果是否可以表明他们在中期及以后的预期结果。本月AJSM的另外两项研究分析了术后早期结果与长期结果之间的相关性。首先将患者分为术后1年mHHS变化中位数以上和以下的组。在术后5年,评分高于1年中位数变化的组的翻修手术率较低,PROM评分较高,并且更有可能达到MCID和PASS水平。在第二项研究中,Shapira等对911名初次接受髋关节镜检查的患者进行了多变量分析,发现术后1年的mHHS评分与是否需要进行关节镜翻修或转换为关节置换术之间存在关联。作者发现,这些患者中有113名(12.4%)在手术后平均约3年接受了其中一种二次手术。作者构建了受试者工作特征曲线,计算出术后1年mHHS>80.5的患者在研究期间接受进一步手术的可能性降低了74%。
21世纪的前20年是髋关节镜检查快速发展的激动人心的时期。正如我们很幸运有这么多有创造力的外科医生开发新技术或改进现有技术一样,我们也很幸运有这么多外科医生和科学家愿意付出辛勤工作来记录他们的成果,以确定哪些有效,哪些无效。不用说,任何研究设计总是有改进的余地。尽管如此,开展一项多中心国际试验所需的计划、组织和勇气,就像FIRST研究小组本月与我们分享的那样,是鼓舞人心的。将这样的研究形象化并贯穿始终,就像耐心地种植一棵树苗一样。
原文阅读:
If a newspaper reporter asked me to identify the biggest stories in orthopaedic sports medicine over the first 2 decades of the 21st century, I'd have to give the lead to the enormous growth of hip arthroscopy and associated jointpreserving techniques. Only 20 years ago, you probably could count on one hand the number of North American surgeons known for their expertise in hip arthroscopy, and they arguably would have had the capacity to meet the continent's demand for this technique. Today, hip arthroscopy is still enough of a specialized interest that its practitioners often concentrate on this one joint, but their numbers have grown exponentially throughout the world. Hip arthroscopy has become an indispensable part of an orthopaedic sports medicine fellowship curriculum. The credit for this growth must be shared by the insightful surgeons who identified femoroacetabular impingement (FAI) as a cause of pain and joint degeneration2,7 and those who drew upon their creativity to apply arthroscopic techniques to its treatment. This ingenuity has allowed surgical management of the acetabular labrum to progress from simple debridement to repair to reconstruction in astonishingly rapid succession. A collection of papers in this month's American Journal of Sports Medicine illustrate the variety of contemporary clinical research in hip arthroscopy.
The first of these articles reflects the growth of hip arthroscopy in the 21st century by chronicling the diagnosis and treatment of FAI in Olmsted County, Minnesota, from 2000 to 2016.10 This county, which had a population of 144,260 in 2010, has the good fortune to be the home of the renowned Mayo Clinic and the Rochester Epidemiology Project. This venture links the medical records of all Olmsted residents, regardless of where they obtain their health care. The authors of the current study identified 1893 patients from 14 to 50 years old who received a diagnosis of hip pain, hip impingement, or hip joint disorder from an Olmsted physician between 2000 and 2016. After examining the patients’ records and radiographs, the investigators determined that 813 hips of 716 patients fit the Warwick criteria for FAI.9 Over the entire period, the incidence of FAI was 54.4 per 100,000 person-years: higher in females (73.2) than males (36.1). An important observation was that the incidence of the diagnosis increased over time, from 40.3 per 100,000 person-years in 2000-2004, to 45.3 in 2005-2009, to 72.6 in 2010-2016. As the authors observe, the most likely explanation for the apparent increase of FAI is a growing recognition of the condition rather than a true explosion in its occurrence. Although nonoperative therapy was the most common treatment, the frequency of surgical treatment increased concomitantly during the study period. Most remarkably, the use of arthroscopic treatment increased from 1 case in 2000-2004 to 160 cases in 2010-2016.
Just as the recognition and treatment of FAI and other hip disorders have matured over the last 2 decades, associated research has flourished. Early reports were typically case series with surprisingly brief follow-up, as practitioners strove to get their initial results into print. In recent years, these have yielded place to comparative studies with 2, 5, and even 10 years' follow-up. Randomized trials are now appearing with increasing frequency. In this issue of AJSM, members of the FIRST investigators group report the 2-year results of an ambitious multinational trial aimed at determining whether osteochondroplasty provides an additional benefit to patients undergoing arthroscopic labral treatment for painful nonarthritic FAI.6 The investigators randomized 220 patients between a control group, which received arthroscopic lavage and labral repair as needed, and an osteochondroplasty group, in which bony cam and pincer impingement lesions were resected in addition to labral repair.
The results of this study may provide an insight into the pathogenesis of acetabular labral injury. When the authors analyzed the planned primary outcome of visual analog scale (VAS) pain measurement at 12 months postoperatively, there was no significant difference between the treatment groups. Secondary outcomes of 12-month functional scores were also not different, with the exception of one score in favor of the control group. However, the rate of reoperation at 24 months, primarily for pain or labral reinjury, was significantly lower in the osteochondroplasty group (8/105) compared with the controls (19/104): odds ratio, 0.37 (95% CI, 0.15-0.89).6
Because there was no difference in the pain level reported by both groups at 12 months, we may deduce that initial pain relief after arthroscopic treatment of FAI may be attributable to the effects of labral repair and lavage. The increased rate of reoperation in the control group, detectable as early as 2 years postoperatively, may be interpreted as indirect evidence that the bony abnormalities characteristic of FAI predispose to the painful labral injury and that this labral damage may tend to recur if the underlying bony lesions are not corrected at the time of surgery.3,21,24,25 A discrete element analysis of hips from 10 patients with cam FAI in this issue of AJSM supports this theory.24 These authors calculated increased peak joint contact stresses during simulated impingement testing in the hips with cam deformities compared with control hips. After adequate cam resection, the peak contact stresses returned to a normal range.
This interpretation of the FIRST trial results is supported by another recent AJSM publication by Domb et al.4 In that retrospective cohort study, the authors divided hip arthroscopy patients into 3 matched groups according to their pre- and postoperative alpha angle measurements: those whose alpha angle was 50° both before and after surgery, those whose alpha angle was .55° before surgery and 50° afterward, and those whose alpha angle was .55° both before and after surgery. At the time of surgery, both groups with elevated preoperative alpha angles, which averaged 66°-69°, were noted to have more labral and acetabular cartilage damage than the third group, whose mean preoperative alpha angle was only 50°. When followed up a minimum of 2 years after surgery, the group whose elevated preoperative alpha angle was not corrected at surgery was less likely to achieve the patient acceptable symptom state (PASS) for the modified Harris Hip Score (mHHS) and more likely to progress to arthroplasty than the other 2 groups.
Just as this study by Domb et al focused on correction of femoral morphology, another study in this month's AJSM by Johannsen et al12 examined how surgical modification of acetabular morphology may have influenced the eventual results. In this study, the authors report the minimum 5-year postoperative outcomes in 192 patients who underwent acetabuloplasty and labral repair. Patients were classified according to the depth of acetabular resection, measured by the change in the lateral center-edge angle (LCEA) and by the magnitude of the postoperative LCEA. In contrast to the Domb study, this group of authors found that these measurements of change in acetabular morphology had little to no relationship to the clinical results as defined by patient-report outcome measures (PROMs) or revision rate a mean of 6.5 years after surgery. This is not necessarily a contradiction, as the Domb et al study looked at the possible effects of underresection, whereas the Johannsen et al study focused on measurements that might reflect overresection. Logically, there must be a degree of overresection of the acetabulum that would adversely affect patient outcomes, but the authors apparently avoided such excessive acetabuloplasty, at least as detectable by the outcome measures chosen. Finally, as the authors note, LCEA is the most common metric of acetabular morphology but may be an oversimplification of the complex acetabular factors that can influence stability or impingement.
These 2 studies aimed to determine how the particulars of the surgical procedure might affect the ultimate treatment results. Much additional clinical hip arthroscopy research has sought to identify other factors that might predict surgical outcomes, including general patient characteristics, preoperative hip anatomy, and preoperative or early postoperative pain or PROM levels.5,11,13,17-20 Most of these studies have been retrospective in design, so they identify associations that would need to be verified as truly predictive in future prospective studies. As New York Yankee great Yogi Berra is reported to have said, "It's tough to make predictions, especially about the future."
Four papers in this month's AJSM examined possible associations between patient characteristics and subsequent surgical outcomes. In the first of these, Menge et al17 reported the results in a cohort of 60 adolescents following arthroscopic treatment of FAI with an associated labral repair. At 10 years postoperatively the investigators noted a 10% revision rate, all cases of which involved female patients, that was significantly associated with global laxity and preoperative symptom duration. In a second study, Lin et al13 report 71% 5-year survival in 109 patients, with failure defined as revision surgery or progression to arthroplasty. When they divided their patients into cohorts aged 15-34, 35-50, and 51-75, the investigators found that the oldest group was 5 times more likely to progress to arthroplasty.
Besides age, Lin et al also found an association between patients' body mass index (BMI) and the Non-Arthritic Hip Score (NAHS) and mHHS at 5 years. A third paper in this month's AJSM, by Parvaresh and colleagues,20 focused specifically on the relationship between patients’ BMI and the 5-year results of arthroscopic treatment of FAI. The investigators divided 140 patients into subgroups of normal, overweight, obese, and morbidly obese according to standard definitions. Although all BMI groups saw a significant improvement in their pain levels, the morbidly obese group was less likely to achieve the minimal clinically important difference (MCID) for PROMs, and all 3 heftier groups were less likely to achieve the PASS and Substantial Clinical Benefit (SCB) than their normal BMI counterparts. The fourth study in this set, "Predictors of Clinical Outcomes After Hip Arthroscopy" by Domb et al,5 also found age and BMI, among other factors, to be associated with 2- and 5-year outcome scores and conversion to arthroplasty in a series of 860 patients.
Aside from examining general patient characteristics such as sex, global laxity, age, and BMI, many studies have been carried out to identify aspects of hip joint anatomy that correlate with surgical success or failure.8,14-16,22 In another study in this month’s AJSM, Maldonado et al14 examine the possible effect of preoperative acetabular overcoverage on the results of arthroscopic treatment for FAI. The authors compared the results in 45 patients whose preoperative LCEA was .40° with a similar number of patients matched for age, sex, BMI, and length of follow-up but whose LCEA measured between 25° and 40°. At 5 years after surgery, both groups had similar average improvements on several PROMs and similar rates of achieving MCID. Interestingly, the overcoverage group actually had a lower rate of conversion to arthroplasty, although the authors concede this might be a type I error attributable to the relatively small size of their groups.
Maldonado and many of the same authors also performed a study comparing 20 patients with borderline hip dysplasia, defined as an LCEA between 18° and 25°, with 61 matched controls whose LCEA measured between 25° and 40°.15 In this study, the patients were undergoing revision surgery and the follow-up was only 2 years. Again, both groups reported similar improvement in PROMs, but the control group had higher rates of achieving the MCID on 2 of the 3 PROMs recorded. There were also differences in the rate of additional revision arthroscopy and conversion to arthroplasty of magnitudes that would be clinically important but were not statistically significant with the sample size studied.
Both patients and surgeons would like to know whether their early results after hip arthroscopy might indicate what outcomes they could expect in the medium term and beyond. Two other studies in this month’s AJSM analyzed correlations between early postoperative results and longer term outcomes. The first divided patients into groups that scored above and below the median change in mHHS 1 year after surgery.1 At 5 years postoperatively, the group that scored above the median change at 1 year had a lower rate of revision surgery, had better PROM scores, and were more likely to achieve MCID and PASS levels. In the second study, Shapira et al23 performed a multivariable analysis of 911 patients with primary hip arthroscopy and found an association between the mHHS score 1 year postoperatively and the need for revision arthroscopy or conversion to arthroplasty. The authors found that 113 (12.4%) of these patients underwent one of these secondary procedures an average of about 3 years after surgery. Constructing a receiver operating characteristic curve, the authors calculated that patients whose 1-year postoperative mHHS was >80.5 were 74% less likely to undergo further surgery during the study period.
The first 2 decades of the 21st century have been an exciting time of rapid evolution in hip arthroscopy. Just as we are blessed to have so many inventive surgeons developing new techniques or refining established ones, we are also blessed to have so many surgeons and scientists willing to put in the hard work to document their outcomes, to determine what works and what does not. Needless to say, there is always room for improvement in any research design. Nevertheless, the amount of planning, organization, and grit needed to carry off a multicenter international trial like the one that the FIRST Investigators group shared with us this month is inspirational. To visualize such a study and see it through to completion is akin to planting a sapling and patiently.
文献出处:Bruce Reider. Hips 2021. Editorial, Am J Sports Med. 2021 Jan;49(1):21-24. doi: 10.1177/0363546520977832.



 京公网安备11010502051256号
京公网安备11010502051256号